Last winter’s sports season had just begun, and the epidemiology staff at Nevada’s second-largest health district were busy calling the parents of high school athletes who’d tested positive for COVID-19.
A state mandate required unvaccinated or traveling athletes to get tested weekly. A nasal swab for an on-site antigen test produced rapid results in 15 minutes; a second swab was sent to an out-of-state laboratory for a more sensitive PCR test. Parents of students who tested positive on the rapid tests would get phone calls from the health district.
Because families already knew about positive rapid results, the phone calls should have been a routine follow-up to start tracking anyone who had had contact with the infected person. But for some reason, parents were repeatedly disputing that their children had the virus.
“These parents were pretty adamant that their kid was not a case and that they could play,” said Heather Kerwin, epidemiology program manager for the Washoe County Health District.
A pattern emerged. Athletes would test positive on the rapid test. But before a contact tracer could call, parents would learn from the testing company that their children’s PCR tests, typically the gold standard of COVID-19 testing, were negative, even for students with symptoms. Kerwin investigated and learned the University of Nevada Reno campus was seeing similarly conflicting results.
The university and school district had something in common. Both had recently hired the same company to conduct their testing: Northshore Clinical Labs.
The Chicago-based company was aggressively pursuing government customers in Nevada. In fact, as Kerwin was learning about the inconsistent results, Washoe County Assistant Manager David Solaro was negotiating with Northshore to provide testing for public employees and local residents. Kerwin thought county officials should know there might be a problem with the company’s tests, and encouraged her contact at the school district and her boss, COVID-19 Regional Operations Chief Jim English, to alert Solaro before an agreement was finalized.
Solaro signed the agreement anyway.
“Why did this go through without a discussion of their discordant results? This is going to cause absolute mayhem,” Kerwin wrote English when she learned the agreement had been signed.
English wrote back: “I tried. No one listens to me sorry.”

Screenshot highlighted and redacted by ProPublica
Kerwin’s instincts were right. As state scientists would later verify, something “catastrophic” was wrong with Northshore’s PCR tests.
A ProPublica investigation into the company’s operations in Nevada, including a review of more than 3,000 pages of internal emails obtained through public records requests, shows the Chicago laboratory’s testing was unreliable from the start. As evidence mounted that Northshore was telling infected people that they had tested negative for the virus, government managers in Nevada ignored their own scientists’ warnings and expanded the lab’s testing beyond schools to the general public.
Ultimately, state public health officials found that Northshore’s PCR tests missed 96% of the positive cases from the university campus — errors that sent people infected with COVID-19 back into the community. But to date, neither state nor county health officials have alerted the public to the inaccurate tests.
ProPublica’s investigation also found that Northshore used political connections, including contracting with the sons of a close friend to the governor, to fast-track its state laboratory license application and secure testing agreements with five government entities in the state. Those agreements not only gave Northshore the exclusive right to test and bill for thousands of people a week, they also gave its lab a legitimacy lacking among upstart testing companies that had set up shop in strip malls and parking lots across the country.
In mid-January, when state regulators finally launched an investigation into Northshore, they found the company had been operating unlicensed sites across Nevada. They allowed the company to continue its rapid antigen testing anyway.
Northshore, which said it had operations in more than 20 states, pitched free COVID-19 testing, telling local officials the tests would be paid for by individual insurance plans or a federal government program for the uninsured. But emails reviewed by ProPublica raised serious questions about the company’s billing practices.
In its pitch emails, Northshore told multiple government agencies it planned to bill the federal program for the uninsured even for those who might have insurance but declined to provide the information. In one case, a Washoe County School District official said in an email the company recommended insured individuals withhold their insurance information so the company could bill the government instead.
As of May 5, the company had collected nearly $165 million from the federal government, 11th most among more than 28,000 companies nationwide seeking reimbursement for testing uninsured individuals.
Northshore, through the public relations firm Weber Shandwick, repeatedly declined requests for interviews. After ProPublica provided the company with a summary of its findings, a spokesperson asked for additional time to address them, then responded: “Northshore declines to comment.”
Although demand for COVID-19 tests waned after the initial omicron surge passed, testing remains a key component of President Joe Biden’s pandemic mitigation strategy. What happened in Nevada offers a cautionary tale as local governments search for ways to provide testing through a system that relies on massive government spending to attract companies to meet the demand.
“It’s still a profit-hungry model,” said Alex Greninger, assistant director of the University of Washington’s virology lab. The guarantee of large payouts prompts companies to take on too many clients too quickly, he added: “Most groups get overwhelmed and exceed clinical capacity. Your operations fall apart.”
“I Do Not Understand Why This Lab Gets Preferential Treatment”
Northshore Clinical Labs has been in business for nearly three decades, but its leadership changed in July 2020. It is now run by three men with no apparent clinical laboratory experience and a history of fraud allegations: brothers Hirsh and Gaurav Mohindra and their associate Omar Hussain.
The Mohindra brothers have been involved in a variety of business pursuits unrelated to the medical field. Hirsh Mohindra was a real estate developer and Gaurav Mohindra lists himself on his LinkedIn page as an intellectual property lawyer.
Together they ran a debt collection business until 2016, when the Federal Trade Commission accused them of operating a scheme in which they bullied people into paying off debt they didn’t owe. As part of a settlement agreement, the brothers and a partner surrendered $9 million in assets and were banned from the debt collection business.
Hirsh Mohindra later served time in prison for an unrelated mortgage fraud case. He was released in February 2020, just as the pandemic was beginning and five months before his mother, Meena Mohindra, was listed as the new president of Northshore in Illinois Secretary of State filings.
In 2019, the FTC accused Hussain of participating in a phantom-debt collection ring with ties to the Mohindras’ case. He also agreed to a lifetime ban on debt collection activities and to surrender assets. The Illinois Secretary of State’s Office currently lists Hussain as Northshore’s president, replacing Meena Mohindra.
The Mohindras did not respond to requests for comment. Hussain declined an interview through a spokesperson.
Last year, the company began a dramatic national expansion. In Nevada, it contracted with Greg and Angelo Palivos, brothers with deep ties to both Chicago and Las Vegas, to build clientele and manage operations. Their father, Peter Palivos, is a prolific contributor to Nevada political campaigns and close enough with Gov. Steve Sisolak that the two met regularly in the early days of the governor’s administration. (Peter Palivos also served time in prison on an obstruction of justice charge related to a fraud case in Chicago, though he maintained he was set up by the U.S. Attorney’s Office for not helping prosecutors build a case against former Illinois Gov. George Ryan.)
The Palivoses’ first task was to get the lab licensed in Nevada. They turned to an influential ally for help: Mike Willden, a former director of the Nevada Department of Health and Human Services, who now works for The Perkins Company lobbying firm, run by former Assembly Speaker Richard Perkins. Willden had worked with Peter Palivos on a past health care venture that didn’t pan out.
Willden said he talked with the manager of the state’s licensing office, who explained to Northshore how to submit its application. But when the Palivos brothers thought it was taking too long, Willden called and emailed his contacts in the governor’s office and laboratory licensing bureau — an agency he had overseen as head of DHHS.
Willden told ProPublica he helped the Palivos brothers as a favor and because he thought the company could help address a dearth of testing capacity in Nevada.
“My understanding was there was a license pending, and in this world of testing where it would take three to five days to get results and everybody was calling me frustrated,” Willden said. “I said, ‘Look, here’s someone who can help you with testing.’”
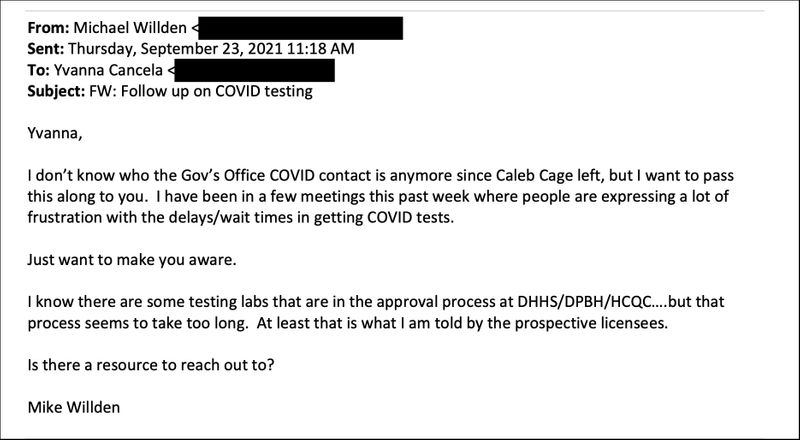
Credit: Screenshot redacted by ProPublica
At Willden’s urging, Sisolak’s chief of staff, Yvanna Cancela, nudged the director of the state’s pandemic response, who nudged the head of the state’s licensing bureau, Cody Phinney. She in turn encouraged the agency to move up its inspection of Northshore’s Nevada headquarters in Las Vegas — much to the dismay of the supervising inspector.
Inspector Bradley Waples would let Northshore skip to the head of the line, but not before complaining to Phinney.
“I want to let you know how frustrating it is to have my staff schedule their inspections only to have labs use previous directors to influence or pressure us into having businesses that they represent, jump ahead of others that are patiently waiting for their inspections,” he wrote.
Waples also noted in his email to Phinney that Northshore would be processing specimens in Illinois, which would delay results. “There are a number of places in Nevada that people can go to get COVID tests in which their results will be available the same day or sooner,” he wrote. “This is why I do not understand why this lab gets preferential treatment while other labs are required to patiently wait.”

Credit: Screenshot highlighted by ProPublica
Three months later, Waples would lead the investigation into Northshore’s testing operations.
In an interview with ProPublica, Phinney said she understood Waples’ frustrations but didn’t view Willden’s request as an attempt to influence the process.
“I didn’t perceive that there was fast-tracking,” she said. “There were questions about when we could get an inspector out there. Certainly, we have staff who are trying to work as fast as they can, and they were being asked to work faster, that’s frustrating.”
Through the agency’s spokesperson, Waples declined to comment.
Willden also downplayed his influence, saying the state was “getting broad pressure to help speed up testing and results. I seriously doubt my inquiries carry that much weight.”
Willden said that he wasn’t paid by the Palivos brothers but that they sent him caramel popcorn and four steaks at Christmas as a gesture of appreciation.
Sisolak spokesperson, Meghin Delaney, said in a written statement the governor has not had conversations with the Palivos family about Northshore’s operations. She said the state’s pandemic response coordinator helped with Northshore’s licensing to avoid a gap in testing service.
“Throughout the pandemic, the State of Nevada has worked to remove barriers and make services available to Nevadans while working through existing regulatory and licensing processes to move expeditiously without cutting corners,” Delaney said. “State employees continue to work tirelessly on behalf of Nevadans, and the State will use lessons learned from across the pandemic to make investments and strengthen Nevada’s public health systems moving forward.”
The Palivos brothers, in a written statement from their spokesperson, Elizabeth Trosper, said they were unaware of the Northshore owners’ history of fraud allegations when they agreed to do work for the company. In addition to generating sales leads for Northshore, Trosper said, their role in Nevada was to manage the local workforce of testers and the collection of specimens.
“They relied on Northshore for standard operating procedures, licensing, compliance, test supplies, molecular lab work, reporting of test results, and billing,” she said.
She said neither the brothers nor their father spoke with Sisolak about Northshore.
“Greg and Angelo Palivos’ involvement with testing was driven by their desire to assist during the COVID-19 crisis,” Trosper said.
“They Make It Sound Almost Too Good to Be True”
When Northshore got its Nevada license in November, it was for a single location in Las Vegas. The company did not complete the paperwork and site inspections required to operate statewide. Still, Northshore began an aggressive push to woo local government agencies across the state. The climate was ripe for what they were offering: free tests.
The delta wave was subsiding and omicron hadn’t yet emerged. But that didn’t mean the need for testing was starting to wane. Quite the opposite.
An OSHA rule mandating large employers to regularly test unvaccinated workers was about to take effect. Universities in Nevada were looking to increase surveillance testing in order to resume in-person learning. School districts were adopting the CDC’s “test-to-stay” recommendation to allow K-12 students who had contact with a COVID-19 case to remain in class if they could produce a negative test. And the governor’s coronavirus plan required regular tests for student-athletes, coaches and others participating in school activities.
That all meant thousands of people would need weekly testing even without a surge of infections. And for each person, Northshore could collect between $165 and $260 for administering the two tests.
At the same time, the Washoe County Health District, a reliable provider of community COVID-19 testing since the start of the pandemic, wanted to focus its testing on communities with less access to health care, such as people without health insurance or a primary care doctor, rather than being the go-to source for the community at large.
Northshore’s pitch was difficult for pandemic-weary government managers to refuse: We can test everyone who needs it on site, we can turn around results in 24 to 48 hours, and it won’t cost you a dime.
“They are very good salespeople,” Kerwin said. “They make it sound almost too good to be true. They hire all the folks. They do it very quickly for you. You don’t have to staff it.”
English, Washoe County’s COVID-19 operations manager, said he was inundated with pitches from labs offering testing. He ignored most of them. But Northshore came recommended by a high-profile doctor who had worked with the district on its COVID-19 vaccination program. English and Kerwin met with Northshore officials and verified they had a state license and could report results through the state’s contact-tracing system.
Then they began referring Northshore to other local governments in the region that were scrambling to find testing resources.
“We didn’t recommend, we referred,” English said. “We told them they had to do their own due diligence.”

Screenshot redacted by ProPublica
Government managers interviewed by ProPublica acknowledged they did only a cursory vetting of Northshore, verifying their license and relying on referrals from people they trusted. They also were swayed by the company’s claims of successful testing operations in other states.
By November, Northshore had agreements with the University of Nevada Reno and the Washoe County School District. By December, Washoe County itself had signed on. In Southern Nevada, the city of Las Vegas signed an agreement for testing in multiple locations, and the city of Henderson allowed the lab to use a parking lot at one of its recreation centers.
Had officials done more research, they would have found Northshore didn’t have the proper licensing to operate statewide.
But government rules that might have ensured a more thorough vetting are suspended during emergencies, such as a pandemic, to allow a more nimble response. More than two years into this pandemic, Washoe County continues to operate under emergency response orders.
Still, Greninger, the University of Washington virology lab’s assistant director, said government managers can take measures to both avoid burdensome bureaucracy and avoid being taken advantage of. For example, they can expand local labs with a documented track record instead of handing out contracts for huge numbers of tests to a single new provider.
“Go to the people with the track record. And try to distribute your risk a little bit,” he said.
“That’s Fraudulent”
Although an attractive sales pitch, Northshore’s promise of free tests was problematic.
The federal government had mandated that insurance plans cover diagnostic testing for COVID-19 ordered by a health care provider and created a fund to reimburse testing of uninsured patients. The law didn’t require insurance plans to cover testing for nonmedical reasons, such as employment requirements, screening for student-athletes and dorm residents or travel. Most major insurance plans do not cover such screening tests, according to Krutika Amin, a policy expert at the Kaiser Family Foundation, a health policy think tank.
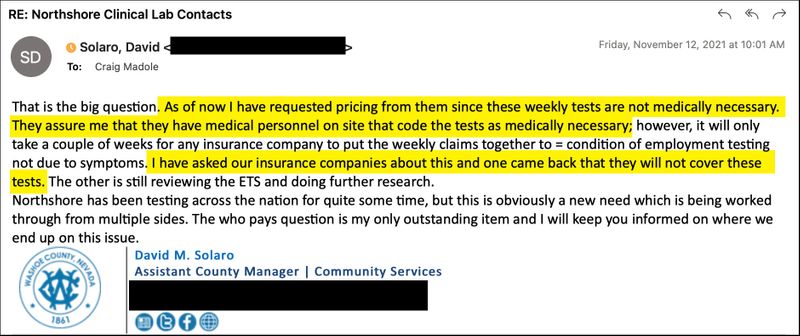
Screenshot highlighted and redacted by ProPublica
Northshore, however, indicated it did not differentiate between the two types of testing in its billing, according to a Nov. 16 email exchange between Northshore’s business development director Razi Khan and University of Nevada Reno officials. The company was relying on a pandemic-specific federal guideline instructing health care providers treating patients to bill for COVID-19 tests as diagnostic tests whether or not the patient had symptoms or could pinpoint an exposure.
“In short, our interpretation” of that guideline “constitutes all COVID-19 testing as clinically necessary and therefore allows for full coverage,” Khan wrote to university officials. He also said Nevada’s positivity rate of 11% justified this billing approach.
Through a spokesperson, Khan declined to be interviewed.
On its registration forms, including for student-athlete screening, Northshore required individuals to sign a statement that they “may have been exposed to someone infected with COVID-19 during my routine daily activities” to be tested.
ProPublica also found an example of Northshore billing an insurance company for a screening test required for a mother and daughter to travel to a high school choir performance. The Reno mother emailed the district after her family’s insurance plan denied the two claims — totaling $470 — because Northshore was an out-of-network provider.
Laura Rich, the executive officer of the Nevada Public Employees’ Benefits Program, which insures most state of Nevada employees, emailed higher education officials after she had been briefed by Northshore on its plans. In the email, she called the practice of billing screening tests as diagnostic “fraudulent.”

Screenshot highlighted and redacted by ProPublica
The Nevada System of Higher Education was considering hiring Northshore to test unvaccinated employees and to provide testing on Southern Nevada college campuses. Rich worried the state employee health plan would be deluged with claims for surveillance tests that it hadn’t budgeted for and was under no obligation to pay. But when she tried to alert decision-makers, Northshore again asked Willden to intervene.
“So I got a call from a certain lobbyist who got a call from Northshore and now I am roped into a meeting with Northshore next week,” Rich wrote in an email to the head of NSHE’s COVID-19 task force.

Screenshot redacted by ProPublica
Rich confirmed that the lobbyist was Willden. She said he didn’t apply pressure, he simply wanted to understand her agency’s concerns with Northshore’s billing practices. But she took from the conversation that Northshore thought her agency was trying to block the company from getting the contract with NSHE.
Ultimately, Rich prevailed in her opposition to Northshore billing the state employee insurance plan for what she believed was surveillance testing. University officials viewed it as unethical, according to the emails, and did not sign a contract with Northshore for the Las Vegas campuses.
Northshore had a backup if insurance wasn’t available: the federal government’s fund for the uninsured.
Documents obtained by ProPublica indicate Northshore planned to bill that fund even for individuals who had insurance. According to Khan’s pitch emails to multiple government agencies, Northshore said it would seek reimbursement from the fund for those who “choose not to provide their health insurance.” Northshore also told the school district it would bill the federal fund if an insurance claim for the test was rejected and recommended the district instruct its employees to withhold their insurance information to avoid claims to its self-funded plan, according to emails from Leslie Allfree, who manages the district’s medical emergency response program.
That contradicts the rules of the program for uninsured patients run by the Health Resources & Services Administration. A spokesperson for the agency said it has safeguards to block testing companies from receiving reimbursement for insured clients, including a database where it can check clients’ insurance status. ProPublica was unable to determine if any Northshore claims were rejected for this reason. As of May 5, the company had been paid nearly $165 million from the fund.
Still, some government managers in Washoe County considered following Northshore’s advice to withhold insurance information on the testing forms.
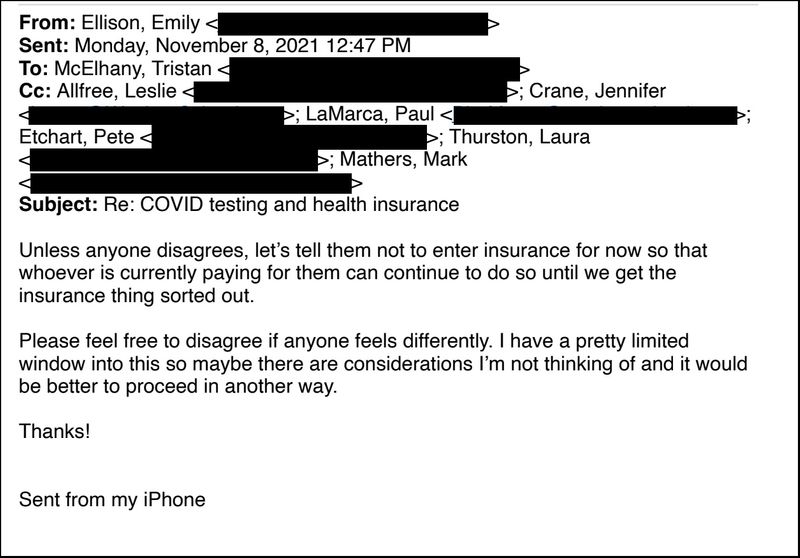
Screenshot redacted by ProPublica
“The vendor recommends that those who are insured by self-insured plans, such as ours, not provide their insurance information and allow the vendor to submit for HRSA reimbursement as if they are not insured,” Allfree wrote. “I foresee messaging around this could be problematic.”
In an interview, Paul LaMarca, the district’s chief strategies officer, said the district did not end up instructing its employees to withhold their insurance information.
Trosper said the Palivos brothers had no responsibility over billing procedures.
“It Is Something Catastrophic”
As officials were debating who to bill for Northshore’s tests, a far larger problem was coming into focus.
The discordant antigen and PCR results at the school district were causing confusion about which students should be kept out of the classroom and which could return.
On Dec. 28, Laura Gingerich, assistant principal at North Valleys High School in Reno, wrote district administrators pleading for them to shut down testing because of the inconsistent results. She had personally tested positive on two rapid tests before receiving negative PCR results from Northshore despite having “every symptom on the checklist,” she wrote.
“I know for a fact this has happened to at least two other student-athletes,” she told administrators. “It is time to stop and question this process. It is not consistent. It is not reliable. We can do better.”
Gingerich did not respond to a request for an interview.
In response, Allfree confirmed the district was “seeing an unusually high number of inconsistent, or what we call discordant results” and was working with health officials to figure out the problem.
The next day, the Centers for Medicare and Medicaid Services cited the Northshore lab in Chicago for deficiencies that put the public in “immediate jeopardy,” including problems with shipping and labeling of patient specimens and inadequate employee training. The problems had affected 1.7 million tests, according to the CMS report.
But word of that investigation did not immediately reach Nevada officials, and Northshore continued signing agreements with local governments. Washoe County could see that the spreading omicron variant was going to require increased capacity. Despite the warnings from Kerwin and the school district about Northshore’s test results, Solaro, the county’s emergency manager, inked an agreement with Northshore to provide drive-up community testing starting Jan. 5.
Solaro said in an interview that the county had to have testing in place for the OSHA mandate, which ended up being struck down by the U.S. Supreme Court, and there were no other options.
“Northshore was in town. They were doing testing for the university and the school district. It seemed like a good move to get them on contract. They needed time to ramp up and hire people. It just seemed like all the right things to do,” Solaro said.
At the time, the concerns about Northshore’s testing were still “anecdotal,” Kerwin later told ProPublica. “I didn’t have any data.”
Data would soon arrive, thanks to a decision by Dr. Cheryl Hug-English, director of the University of Nevada Reno’s student health center. She had noticed contradictory results in the first weeks of testing and contacted Northshore several times looking for an explanation and a solution that never came.
With problematic test results piling up, Hug-English began running an experiment in December. She quietly sent patient specimens to both the lab in Chicago and the Nevada State Public Health Laboratory, which had done PCR testing for the campus prior to Northshore’s arrival. After a month, the results were clear: Northshore’s PCR process wasn’t working. More than 96% of the PCR results that came back positive from the state lab came back negative from Chicago.

Screenshot highlighted and redacted by ProPublica
Kerwin and Hug-English again tried to get answers from Northshore. Kerwin asked if the company was seeing similar problems at any of its other testing sites across the country.
“Oh, no, this is just a weird thing going on in Washoe,” Kerwin said she was told.
“I’m like, science says that’s probably not true. But they weren’t going to be any kind of transparent with us about the real reasons,” she said.
Kerwin asked the state lab to investigate why Northshore’s testing was so unreliable. State scientists exchanged emails with Northshore representatives, and, while they never arrived at a clear explanation, they came away determined that PCR testing from Chicago should stop.
“Without physically being in their laboratory, I can only guess at what is going wrong. But it is something catastrophic,” the state lab’s molecular supervisor, Andrew Gorzalski, wrote on Jan. 10. “My personal recommendation would be to stop using Northshore for SC2 PCR testing immediately.”

Screenshot highlighted and redacted by ProPublica
By that time, however, the mayhem that Kerwin had predicted was erupting. The omicron surge completely overwhelmed Northshore’s operations. Community testing sites had lines so long they snarled traffic. Schools that offered Northshore testing to symptomatic students, families and staff had sick people wandering hallways. So many people needed testing that Northshore testers couldn’t keep up. Angry parents took their frustrations out on school staff.
“This is the second week in a row and tensions are getting to the boiling point with the people we have to turn away,” wrote one high school administrator.
Then Northshore’s employees began to get sick. The company was not providing N95 masks and gowns or requiring staff to wear them, according to emails from the school district and a state investigation. Some testers wore less-effective cloth or surgical masks. Some didn’t wear gloves. So many employees became ill, the company had to suspend operations at two county sites, according to emails from the Palivoses.
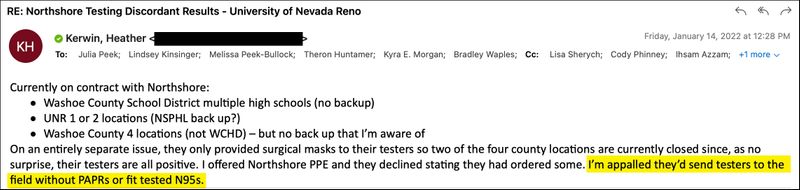
Screenshot highlighted and redacted by ProPublica
In response to concerns from Kerwin and school officials, the company purchased better personal protective equipment.
“We have also bought face shields, N-95 masks, and gowns for our techs to use at their discretion. Effective: 1/17,” Greg Palivos wrote to the school district on Jan. 16.
Trosper said the Palivos brothers stopped PCR testing in January, when the state notified them of the inaccurate results. An email exchange provided by Trosper shows Angelo Palivos had pushed Northshore to fix its problems before it even got to that point.
“This casts more doubt on the efficacy of Northshore lab, in what is already a very fragile situation with plenty of doubt already cast,” Angelo Palivos wrote to Hussain on Dec. 16. “This is very concerning to everyone in Washoe County, and us as well.”
Hussain responded in reference to patients with contradictory results: “They need to be retested.”
Kerwin was fed up with her concerns going unheeded by local officials. On Jan. 14, after the state lab documented the 96% false negative rate, Kerwin emailed state health officials: “I am asking for Northshore’s license for PCR testing in Nevada be revoked immediately.”

Screenshot highlighted and redacted by ProPublica
Even then, state inspectors were slow to act. Worried the school district and community would be left in the lurch if Northshore halted operations, the deputy administrator of the state Division of Public and Behavioral Health, Julia Peek, asked for a backup plan. But there wasn’t one. Peek and Kerwin agreed Northshore should continue using rapid tests while ceasing PCR testing. The rapid tests were accurately “coming up positive,” Kerwin said.
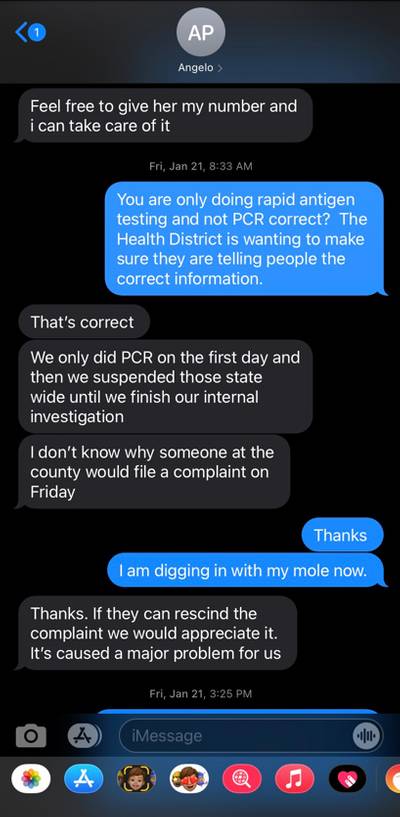
A text message exchange between Northshore’s Angelo Palivos and Washoe County Assistant Manager David Solaro Credit: Screenshot obtained by ProPublica
When it became clear the state would investigate Kerwin’s complaint, Angelo Palivos texted Solaro, at the county, to try to put a stop to it: “If they can rescind the complaint we would appreciate it. It’s caused a major problem for us.” Solaro said he was “digging in with my mole now” to find out who had filed the complaint.
Trosper said Angelo Palivos challenged the complaint because the brothers had already told the testing sites to stop PCR testing.
Solaro told ProPublica he did not uncover who filed the complaint or take any action to have it rescinded. He said Angelo Palivos was frustrated. “In his mind, we needed their help, and here we are filing a complaint,” Solaro said.
At this point, Phinney’s agency, which was responsible for licensing and inspecting the lab, learned about the discordant results and discovered that Northshore was testing at locations across the state despite only being licensed for a single location. Waples immediately sent out an investigator, who came back with a list of deficiencies in Northshore’s operations, including not properly training all of its workers, not following the test manufacturers’ instructions and not properly performing quality control measures.
Waples was reluctant to shut down Northshore’s operations and instead said he wanted to bring them “into compliance.” In an interview, Phinney said that’s common practice for the bureau. “When we have a facility or provider that appears to be working with us, we do our darndest to work with them.”
By February, demand for testing had dropped. Although Northshore provided investigators with 600 pages of documentation to support its claim that it had fixed the problems, regulators continued to find deficiencies. In the end, Northshore decided to abandon its operations in Nevada and asked for the agency to close its license.
At this point the Palivos brothers also ended their relationship with Northshore. Trosper said Northshore still owes the brothers “hundreds of thousands of dollars” for employee salaries, subcontractors and vendors.
Ultimately, the state of Nevada rescinded the license and closed its investigation, but not before detailing its findings in a letter to the company. The director of the state Department of Health and Human Services, Richard Whitley, wanted the issues to be documented.
“It’s like staff who do harm and we let quit rather than be fired and then there is no record of the performance and they can reinvent themselves after a period of time and come back,” he wrote to Phinney. “We shouldn’t let this happen in health care.”

Screenshot highlighted by ProPublica
Republished with permission from ProPublica, by

ProPublica
ProPublica is an independent, nonprofit newsroom that produces investigative journalism with moral force. They dig deep into important issues, shining a light on abuses of power and betrayals of public trust — and they stick with those issues as long as it takes to hold power to account.
With a team of more than 100 dedicated journalists, ProPublica covers a range of topics including government and politics, business, criminal justice, the environment, education, health care, immigration, and technology. They focus on stories with the potential to spur real-world impact. Among other positive changes, their reporting has contributed to the passage of new laws; reversals of harmful policies and practices; and accountability for leaders at local, state and national levels.
